Top > About Us > News Letter > “Palliative care” in the future
“Palliative care” in the future
Special Topic Medical care along with cancer treatment
In many cases, palliative care has been provided as part of end-of-life care.
From now on, however, palliative care can start anytime once cancer is diagnosed, not only in the end-of-life phase. Our hospital is actively working on providing this care.
Palliative care starts once cancer is diagnosed
Many cancer patients in the terminal phase are known to suffer from pain; however, it is known that ~20% of cancer patients, for whom curative treatment is still available, suffer from chronic pain. Palliative care for cancer patients aims to relieve their physical and psycho-psychiatric symptoms caused by both “cancer itself” and “cancer treatment” (e.g. pain, dyspnea, nausea, anxiety, and depression), and it is based on the concept of respecting the life and personality of cancer patients. Once they are diagnosed with cancer, these patients can receive palliative care along with cancer treatment at any condition or stage, not only in the end-of-life phase. Starting palliative care as early as possible enables us to provide better medical care regarding cancer treatment, which leads to an increased possibility of radical cure of the cancer, stronger prevention of a life-threatening condition, and sustained rich quality of life. We are designated as a cancer care hub hospital. A role of the palliative care team in this hospital is to relieve patients’ physical and psycho-psychiatric symptoms related to their treatment and to assist the attending physicians in charge of treating cancer, so that they can provide the patients with medical care that is best for the patients. This concept is well accepted overseas, but it is not widespread in Japan. In our hospital, therefore, we are actively engaging in spreading the concept widely in the “Pain Clinic in the Cancer Treatment Phase” that was opened last year. Once cancer is diagnosed, the palliative care team participates in a patient’s treatment to take measures against side effects caused by cancer treatment, as well as against pain caused by cancer. In the end-of-life phase, we are also making an effort to relieve physical and psycho-psychiatric symptoms so that the patient and their family can make a peaceful end.

The palliative care team in this hospital
Palliative care team in multidisciplinary collaborative work
The palliative care team in this hospital consists of physicians (anesthesiologists, hospice doctors, psychosomatic internal physicians, psychiatrists, and radiologists), nurses (certified nurse specialists in cancer nursing and certified nurses in palliative care), pharmacists, and clinical psychologists. By having these healthcare professionals with different medical backgrounds and merging their individual expertise, we aim to provide better palliative care. Inpatients are visited by the palliative care team. By having four conferences weekly, each member of the team accurately understands the condition, which may change on a daily basis, of all patients who receive palliative care.
The palliative care team also cooperates with other departments and specialized teams. Multidisciplinary conferences that are organized mainly by the palliative care team have various participants, including nurses and social workers in the Department of Medical Community Network and Discharge Planning as well as physical therapists and occupational therapists in the Rehabilitation Center. At these conferences, we assess whether the care environment is appropriate for a patient’s condition, and we aim to provide medical care to comprehensively support the patient. In addition, because patients in the end-of-life phase often pass away in a local hospital near home or at home, we support their decision about where they would like to die in cooperation with the Department of Medical Community Network and Discharge Planning, with the aim of making the care environment peaceful. Furthermore, we have been improving the provision system of palliative care in the entire hospital by carrying out educational activities to give hospital staffs a better understanding of palliative care through the Cancer Board, which consists of physicians, nurses and pharmacists who are responsible for actual cancer treatment.
For patients whose pain is resistant to analgesic medications
Narcotic analgesics are very important drugs to improve pain from cancer patients. Overdosage, however, can trigger serious side effects. One of the missions of the palliative care team is to make adjustments to provide an appropriate dose of a narcotic analgesic. Pain control that starts from the initial cancer treatment phase may last for a relatively long time. Because our hospital has broad experience in chronic pain treatment, we can provide high-quality medical care to treat pain in cancer patients. We also opened the “Second Opinion Clinic of Palliative Care for Cancer Pain” last August to provide expert opinions to patients whose pain is difficult to control by palliative care in other medical institutions.
Although narcotic analgesics are generally used against pain in cancer patients, they cannot completely eliminate pain in some cases. In this hospital, we provide “spinal cord stimulation therapy”, which is usually used for neuropathic pain or ischemic pain, to treat cancer pain in patients for whom analgesic medications are not effective. In some cases, however, to provide this treatment, temporary discontinuation of cancer treatment may be required. For the spinal cord stimulation therapy, an electrode is inserted into the back near the spinal cord (nerve fascicle). A battery is separately implanted into the body, similarly to a pacemaker to treat arrhythmia. When a patient feels pain, the patient operates an external remote controller to generate electrical stimulation to the spinal cord. This triggers a comfortable sensation like being electrically massaged from inside the body, which relieves the pain. Unless complications occur after the implantation surgery of the devices, such as an infection or internal bleeding, there is basically no side effect. In addition, there is no limitation on daily usage, unlike the use of analgesics.
Incorporate exercise
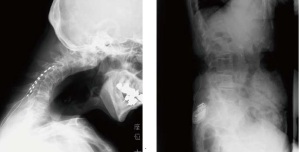
A lead (left) and a stimulator (right) that were implanted into the body for spinal cord stimulation therapy
Data from many international reports show that exercise in addition to standard cancer treatment results in a lower recurrence rate, and that patients with an exercise habit experience less side effects caused by chemotherapy (these effects vary depending on the type of cancer). These data indicate that incorporating exercise at the starting stage of cancer treatment may relieve side effects that will occur during the future treatment, even if the patient did not have an exercise habit previously. At the Pain Clinic in the Cancer Treatment Phase, therefore, we also provide instructions on exercise as needed. In addition, a device to support exercise at home has been developed mainly by Dr. Masahiko Sumitani, the Director of the Department of Pain and Palliative Medicine. In this system, an exercise example and a patient’s actual movement are displayed together on a monitor; therefore, a patient can exercise while confirming whether they are moving correctly as instructed on the monitor. Furthermore, a patient’s exercise data will be received by physicians in the hospital and will be used for medical care. We aim to put this device to practical use in the near future. Another device for a patient with a paralyzed part of the body has also been developed – a patient wears the special device to increase their muscle strength.
| In this hospital, palliative care by the palliative care team is available during cancer treatment. If you would like a consultation, please ask your attending physician or nurse. |
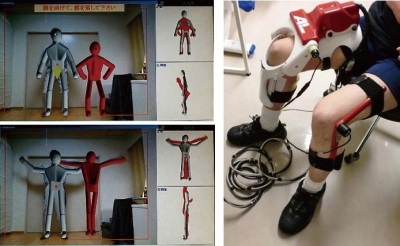
A home exercise device under development
(a patient exercises according to instructions on a monitor (top left). An exercise example and a patient’s actual movement can be compared on the monitor (bottom left). A patient with a paralysis can wear a special device for muscle exercise (right)).
